Caring friends in my circle cautiously ask me how I am. I do appreciate their concern. The fact that I am in their thoughts is comforting to me.
When they ask, almost everyone says, “You look great!” to which I reply, “Thank you, that’s really all I care about.”
(It’s true. My vanity prevails. Yes, I’m that shallow. Since the diagnoses, and even through the Bald Period, my deepest fear wasn’t dying of cancer–it was looking like a cancer patient.)
Then I tell my friends the most important things about my current condition:
First, I am grateful for all of the love in my life–my friends and family and communities that have sustained me since my first primary diagnosis.
Second, I am grateful for all of my abilities.
And that’s where I usually leave it, because the full story is just depressing.
My family and closest friends are well aware my current challenges.
I’ve been in remission since June 22, 2014: cancer-free, for now. I like being in remission. It’s a nice place to be after so much drama.
While I am doing everything I possibly can to stay healthy, the truth is, it’s a crap shoot. Advanced stage cancer has a nasty habit of recurring.
Fortunately, I am comfortable living with uncertainty. In fact, I’m kicking cancer’s ass by living well. (And everyone can learn to live more fully by watching Stuart Scott’s stunning speech accepting the Jimmy V Award for Perseverance in July 2014. Every word is true. Sadly, he died less than six months later.)
Almost two years since my dual diagnoses of advanced stage breast cancer (March 2013) and spinal cord compression (May 2013), I expected to have recovered or nearly recovered.
Reality: the side effects of chemotherapy and spinal cord compression persist and interfere with my ability to function. The gap between where I expected to be and where I am plagues my consciousness.
The subject is often the focus of my sessions with the phenomenal psychotherapist, Barbara Brown.
My phenomenal family doctor, Debbie Honickman, recently told me I need to work on “the acceptance piece.”
When I relayed my discussion with Debbie to my close friend (and Emily’s father), Stephen Parkinson, he defined acceptance: “It means not wishing things were different, or better.”
I’m still trying to fit this definition into my worldview. It’s not easy.
Here’s the list of issues, in no particular order:
My brain:
Some chemotherapy drugs cause “chemo brain” or “chemo fog,” a temporary cognitive deficit that can last up to two years. It has been postured that I may have a nasty case of it because emergency spinal cord surgery interrupted my chemotherapy treatment. Before healing completely (basically, once I could walk without assistance), I returned to chemo. My neurosurgeon, Michael Fehlings, told me that chemotherapy is a disaster for the nervous system. “Where do you think chemo brain comes from?”
When tested in my youth, I had an IQ of 141. Today, it hovers around room temperature (Fahrenheit). At least it feels that way.
Having no short-term memory is terrifying. I don’t remember a conversation I had yesterday, what I did yesterday, or even if I have eaten. I determine whether I’ve had breakfast by looking for evidence in the dishwasher. (My disconnect with my stomach will be explained later.) Sometimes during a conversation, I lose the subject. I am awash with shame and humiliation.
Aside from memory, I struggle with organization, cause-and-effect relationships and even simple problem-solving. For example, just over a month ago, when planning the annual Chanukah Party for my staff, I was quoted three latkes for five dollars. I spent twenty minutes with a calculator, then my fingers, trying to figure out how much 50 latkes would cost. I was sweating. I could feel my blood pressure climbing. “Dear god,” I thought, “this is simple arithmetic.” I gave up.
The chemo fog may be exacerbated by chemo-induced menopause. However, my condition goes far beyond difficulty retrieving nouns.
Coping strategies for my brain
I write everything down. If I don’t, it’s gone from my head. I live by lists. I have lists of lists, in fact, including lists of rules that allow me to function and to keep me from falling apart.
Here’s an example:
If I find myself without paper, I write on my hand or my arm. I find myself re-reading the previous chapter of a novel from where I left off, because I don’t remember what I’ve read.
I am Guy Pearce in the film Momento. There are Post-It notes everywhere. I should have a Polaroid camera.
I am handfuls of supplements, daily self-massage (myofascial, lymphedema, feet), trips to the gym, foot exercises, weekly Vitamin C infusions, mistletoe injections (three times a week) and endless rules: the keys always go on the hook, the credit card always goes back in the wallet, eye glasses always in my purse, meds always always go in the Med Cupboard, appointments/dates always go in my iPhone calendar. And now, I have a paper calendar as a back-up.
The list of rules is endless. In spite of this, I occasionally stand up friends inadvertently, or I present at the wrong clinic for an appointment, or show up on the wrong day. Welcome to my life.
Anxiety of cognitive issues definitely exacerbates the fog. Following advice from Debbie and Barbara, and also my Traditional Chinese Medicine practitioner, Angela Warburton, I acknowledge my limitations and remind myself it’s temporary. I try not to chastise myself.
My feet
When the joints in my feet became painful about a year ago, my medical oncologist, Eitan Amir, suggested it was from the Tamoxifen, something of a miracle drug that blocks estrogen receptors and helps prevent or delay breast cancer recurrence. One of the many potential side effects is joint pain.
My dear friend, Ellie Goldenberg, had re-introduced me to the joy of dance in December 2013. It was a form of healing, a spiritual therapy. But by the summer of 2014, the pain was unbearable. I could barely walk. I had to give up dancing.
Before stopping the Tamoxifen, however, I wanted to rule out the possibility that the pain in my feet was something unrelated to cancer treatment. So I booked an appointment with my son’s chiropodist, Chance Ng, at the Bathurst Foot and Ankle Clinic.
First, I told Chance about my medical history and the peripheral neuropathy. After examining me and testing superficial and deep tissue sensation, he informed me, “You have no sensation in your feet.”
“I know,” I told him. That’s how I had started the conversation.
“Because you can’t feel anything, you’ve been placing your weight on the wrong parts of your feet when you walk.”
So, the excruciating pain in my feet had nothing to do with cancer treatment.
Then he told me, “All of the muscles in your feet have atrophied, and every joint in both feet is inflamed.”
I had a severe case of both plantar fasciatis and metatarsalgia. To complicate matters, my feet have a very rare shape. Chance called it a congenital deformity.
At least we have a diagnosis and a treatment plan. First, he created splints for my shoes to test a proposed shape for the orthotics. After a two weeks, the splints were flattened. He made them higher. After another two weeks, he cast my feet for the orthotics. I was also to ice my feet, rub Voltaren into all of the joints twice a day, stretch my calf muscles and sleep with a leg splint. The pain in my feet went from a 9 out of 10 to a 6 out of 10.
Today, I can walk or stand for about 10-15 minutes before my feet feel as though they are on fire. It’s a huge improvement!
I am working now on making a connection between my brain and the muscles in my feet. It’s not easy.
I look forward to when I can dance again.
Coping strategies for my feet:
Cycling is pain free, fortunately, and I was able to get back on my bike 14 months after spinal cord surgery.
I do not hesitate to use seating for people with disabilities or, wherever I am, to ask for a seat.
At parties, I will stand for up to 10 minutes, then I sit. Sometimes I sit alone, and that’s ok.
It should be noted, I choose not to take pain medication. My body is a toxic waste site; I don’t need any more crap inside me.
My head and neck
Because the first three vertebrae of my neck were fused, with some rather elegant hardware, I have limited rotation. It’s a lot better than it was a year ago, though.
Every afternoon, usually between 2:00 and 4:00, my entire head goes numb, and my neck starts to ache. This is my body telling me to lie down. It’s not just fatigue (also a feature of chemo brain), but my head is just too heavy on my neck.
By lying down for 30-60 minutes, the neck pain becomes manageable, and I am able to be up and about until after dinner.
By the evening, however, I have to be horizontal. If there is a late-night event, I will have a rest for about an hour beforehand and stay up for as long as I’m comfortable.
Coping strategies for my head:
My friends are quite used to me spontaneously crashing in the spare bedroom or, sometimes, in their bedroom, and they will help me move me to the couch when the party is over.
I always have a toothbrush and my meds on me.
My numb hands and feet
I had surgery on my spinal cord in July 2013. The numbness in my arms, hands, legs and feet caused by spinal cord compression persists, 18 months after surgery.
Aside from my aching feet, I have balance issues.
I used to fall a lot, really wipe out, particularly when there was an unevenness in the sidewalk. (It sounds so much better in Spanish, “disnivel,” or Italian, “disnivelo.”) My jeans or stockings rip, I’m bleeding in at least two places, I need someone to help me up.
Between September 2013 and June 2014, I fell down a flight of stairs five times, in spite of holding onto the banister. My hand isn’t strong enough to support my body when my feet give out.
The beautiful thing about peripheral neuropathy, though, is that you don’t feel a thing! Every time I fell down the stairs, I would stand right up. Amazing, I thought, I didn’t hurt myself. Only later to find a massive hematoma on my ass or, when later I notice dried blood on my foot, a missing toenail.
Similarly, my hands do not function as they should. Sometimes it’s hard for me to hold a pen, much less write legibly. I make mistakes keyboarding. Texting is a chore.
Again, I don’t feel pain in my fingers. When cooking, for example, I know that I’ve cut myself only when I see blood on the onion. (I regularly cut the lymphedema arm. Not good!)
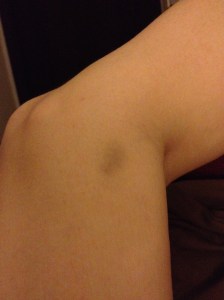
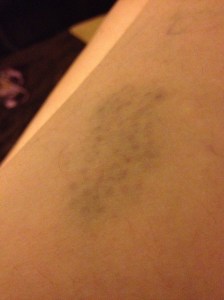
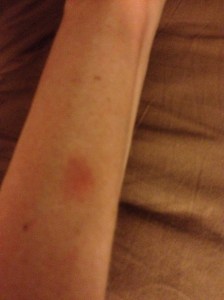
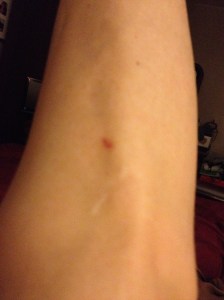
I also bump into things without realizing. My myofascial therapist informs me of the bruises on the backs of my legs. Again, no pain.
Occasionally, I take a photographic inventory of lesions–the ones I can see. Here is an example:

Hard to see, but the circulation of my second toe was cut off for hours because of a hole in my panty hose. I didn’t feel it.
Coping strategies for my numb hands and feet
Rule # 1: JDF – Just Don’t Fall
I move at one speed: slow. I never rush anywhere. I look at the pavement in front of me–always. I hold onto the banister–always.
If I have to walk in the evening, when my feet are at their weakest, I hold onto the arm of the person I’m out with. Sometimes that’s one of my children. Sometimes it’s a friend, or a date.
I do nothing on a bosu.
Rule # 2: PYH – Protect Your Hands
By keeping knives sharp, by cutting slowly, using hand lotion to keep the skin from drying, taking off my rings at night.
Instead of texting, call, FaceTime or Skype.
Break regularly when typing.
My stomach
My gastrointestinal system shut down completely, due to stress. I used to have a stomach like a rock, but all that changed, and it took months for me to figure out why.
In February 2014, immediately after my treatment had finally ended, a radiologist felt compelled to show me a mammogram image: there was a cluster of microcalcifications by the surgical clip, i.e., by the original tumour bed–an early sign of a breast tumour.
I chose to put faith in the fact that the radiation keeps working after treatment. I didn’t realize that the image I’d seen could have a traumatic impact on my psyche, and my body.
Two weeks later, I stopped absorbing food. I won’t go into gory details, but I will share that was a lot of weeping in the bathroom–until I saw my psychotherapist.
Immodium, bismuth, homeopathic remedies had no effect. Over the next three months, I eliminated any possible trigger food from my diet, stopped my medications one at a time to see if that had any effect, and had every test, including a colonoscopy, yet the results were all negative.
As a result, I developed a fear of eating–anything. I developed a disconnect between my brain and stomach. I can’t tell if I’m hungry or full.
Irritable bowel syndrome, as my older brother Carl informed me, is one of the stress-related conditions only seen in the West. Other examples are fibromyalgia and chronic fatigue syndrome.
I didn’t see my psychotherapist, Barbara Brown, for several months. (Our travel schedules conflicted.) She pointed out that, after the physical and psychological trauma I’d been through over the past year of surgeries and cancer treatment, it’s normal that some part of my body is going to suffer. It needs time to recover.
In eight months, I’ve lost over 30 pounds, or 20% of my body weight. I weigh less than I did 25 years ago, before I had my first child.
Coping strategies for my stomach
Daily meditation and energy work.
Conversations with my stomach, generally in the tenor of: “Take your time. After all you’ve been through, it will take time to recover. I understand and support the recovery process.”
When I ask my stomach what it needs to tell me, all I get is “Leave me alone.” I interpret that to mean, “Stop focusing on your stomach. It only makes it worse.”
Subclinical depression
In our meeting last month, Eitan Amir suggested that the persisting chemo brain may actually be attributed to subclinical depression.
“I’m not depressed!” I said.
“That’s what subclinical means,” he said. “You don’t have any symptoms. Some times a low-dose antidepressant will help cognition.”
I had no intention of adding another pharmaceutical to my routine, until he said, “It may also help your GI system.”
Then I reconsidered his suggestion. I told him I would talk to my family doctor about it.
He also told me he doesn’t think I have peripheral neuropathy, but central nervous system neuropathy, and he has referred me to a neurologist. (I’m not freaking out because there is no sense worrying until this has been confirmed.)
When Debbie and I discussed the suggestion of a low-dose anti-depressant, she was not in favour of it. “You can do meditation and energy work instead, and the outcome will be the same.”
I’d had four days of not-so-horrible diarrhea, so we agreed to give mindful meditation and energy work for a month and re-visit the issue in January. Although I was still having problems at our next meeting, both of us were comfortable forgoing the anti-depressant.
Conclusion
There are a lot of people in this world dealing with a lot worse.
I’m positive that my cognition will return to normal or near-normal function, and that, with time, my GI system will start functioning again.
As for the neuropathy, it is likely permanent. It’s been 18 months since the surgery, and there has been no change. It means my feet may not improve from current state.
I’m still lucky to be alive.




![IMG_2641[1]](https://elizabethjabraham.com/wp-content/uploads/2015/01/img_26411.jpg?w=300&h=225)


I guess I am like everyone else wishing we could help you and feeling frustrated that we cannot do anything but cheer for you from the sidelines.
Go Elizabeth!
Rick
Sent from my iPad
>
Thank you, Rick! Thanks to your active cheering (and others’ as well), I’m not spending my days in bed under my quilt.
Sending love
xox
Time and life may separate, but the call of the heart is strong. A mutual friend told me and I had to respond. Get in touch. I’m here. Hugs…PJ