Tripping the light fantastic with James Summers on the Norwegian Breakaway, maiden voyage, post-op
To chemo or to cruise…that is the question
Once I recovered from surgery, I knew I would have to start chemotherapy. I only had one small problem: I had a date with my daughter and a Transatlantic cruise – the trip of a lifetime – one month post-op.
I knew that cancelling the cruise, and other events I was looking forward to, would be surrendering to the disease. This was contrary to my nature.
When we met a few weeks after my surgery, I informed my medical oncologist, Eitan Amir, that I was not going to cancel any of my plans.
The Norwegian Breakaway was scheduled to launch from Southampton, England on April 30, 2013 and arrive in New York on May 7. After a brief visit with my parents, the plan was to fly to California, give two workshops to physicians and administrators, then visit my younger brother, Scott, and sister-in-law, Stacy, before returning home.
A week later, I was to fly to Gothenburg, Sweden, to present a paper at a meeting of the Health Promoting Hospitals Network, a partner organization of the World Health Organization Europe.
“You’ll have your first treatment on May 15th, between California and Sweden,” Eitan said.
I like Eitan. He’s an Israeli with a charming British accent, super smart, and straightforward.
“Okay!” I knew I was taking a risk, leaving the country without knowing how I would react to the chemotherapy, but I didn’t know if I would ever have another opportunity to present to this group.
Ironically, two years before the cruise, Emily had suggested that we grow our hair and donate it to one of the organizations that makes wigs for women who have lost their hair to cancer. After my diagnosis, we decided to raise funds for research at Princess Margaret Cancer Centre. Our hair, by that time, reached our respective waistlines.
Until that point, Emily and I had kept my diagnosis private, among family and close friends. During the cruise, we both made the difficult decision to go public. As we read the thoughtful, encouraging messages from family and friends, we knew that we had made the right decision.
Travelling the high seas with Emily and our friends was a magical experience. We bought passes to the Thermal Suite, a steamy, luxurious spa at the front of the 15th deck, with floor to ceiling glass on three sides. We dined and danced with our friends. We soaked in outdoor Jacuzzis.
On the last day, Emily and I daydreamed about finding a place to hide before we docked, so we could stay on the ship forever. Solomon could sneak on when we docked.
My dad, who has been calling me every day since my diagnosis, picked us up at the docks, and we spent the day in the city.
The following day, I flew to California, ran the workshops and visited my brother and sister-in-law. My family is super cool. We are all a bit crazy, in a good way, and we always have fun together. When my dad, the iconic patriarch, gets everyone together, it’s like a circus, in a good way. I am fortunate that everyone rallied around me when I was diagnosed. They are my rocks.
The day after I returned from California, celebrity stylist and my dear friend, Steve Roy, cut Emily’s and my hair. We raised over $2,000.
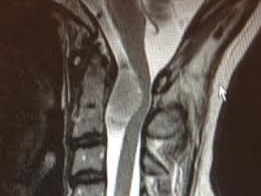
Sporting a new bob, I met with Eitan the day before my first chemotherapy session. He handed me a copy of a report from my full spine MRI. The scan was ordered because a bone scan indicated there may be a problem at T12, perhaps a fracture. The MRI showed no issue at T12, but an incidental finding: there was a 2.4 cm tumour compressing my spinal cord at C1.
“They say it’s critical,” he said, “but I don’t think it will be necessary to interrupt chemotherapy. In any case, I’ll refer you to a neurosurgeon for a consult.” It was booked for the day after I returned from Sweden.
A tumour on my spinal cord, just beneath my skull? Seriously?
The following day, Emily and I packed for chemotherapy as though we were going to a picnic. Sliced mango and papaya, dark chocolate, cards, music, an iPad to watch movies and, of course, Prosecco—anything we could think of to make the road a little smoother.
Our nurse couldn’t have been nicer. She had to administer four tubes of medicine manually, which meant that once she inserted the needle and snaked it up my vein, she literally pushed the fluid into my vein, bit by bit, staring at my arm to make sure the medication didn’t leak into the surrounding tissue. This took about an hour and a half. The last medication was administered with a pump.
Emily and I were so busy talking to—and laughing with—the nurse that we never had time to watch a movie or play cards. Except for the insertion, it was all quite pleasant. We walked to the car together afterwards, and she drove home. Solomon was still at school. We went to a café, then headed for the park, where we sat and ruminated about the experience. I felt completely fine, though exhausted. But so was Emily, and she didn’t have chemotherapy.
The next day, I still felt fine. No nausea, no change in appetite.
The conference in Gothenburg, Sweden was transformative. The theme of the conference was Body and Mind, and one of the streams was psychoneuroimmunology: the impact of mental state on immune response. During the opening plenary session, I felt as though the universe meant for me to be there and hear about this research.
My mental state can influence my immune system. Brilliant! I can get through this. I will get through this.
Gothenburg was also about seeing friends I work with, from Toronto and internationally, who comforted me with stories of survival, hugs and, from one Norwegian colleague, healing teas. At the gala dinner, I danced for hours with health promoters and CEO’s of regional health authorities from Europe. At 2:00 a.m., I had a nightcap on the roof of the tallest hotel in the city.
When I returned from Sweden, I met with neurosurgeon Michael Fehlings at Toronto Western Hospital. He specializes in spinal cord tumours. I had taken Emily with me to be my scribe and later regretted the decision. The news was shocking to both of us.
The fellow who met with us first showed us the MRI on the computer monitor.
The tumour took up most of the space of my spinal canal. My spinal cord was smashed against one side.
“It’s amazing that I have no symptoms,” I said.
The fellow replied, “With this kind of compression, it’s amazing you’re not in a wheelchair.”
She examined me before Michael Fehlings came into the room. After a second examination, Michael asked about my treatment plan, which at that time was a year. Michael didn’t want to wait that long to remove the tumour, which would eventually stop my heart from beating, and my ability to breathe.
He proposed the window between chemotherapy and my next surgery, to remove all of the lymph nodes under my left arm.
“But if you have any symptoms, we’ll have to interrupt chemotherapy.” Emily and I looked at each other. “The first sign of numbness or tingling in your hands or feet, call me.”
After the appointment, stunned, Emily and I ended up at The Drake for brunch, with mimosas.
We agreed not to tell anyone, except my brother, Carl, a physician. Not my parents, not Solomon, or any of my other siblings. It was just too much bad news.
It wasn’t until two weeks after my first treatment, when my hair started falling like rain from my head, that we had proof that the chemotherapy was working.
My medical oncologist had warned me. My family physician had warned me. And Steve Roy. My attempts to manifest keeping my hair through meditation had failed.
Steve cut my hair very short in his home. It was an in-between stage, before it had to be shaved. Emily was there with me.
If anyone else had been giving me a pixie cut, I would have been crying like a baby. But Steve was so compassionate and funny, telling us stories about the women he knows who have been through the same diagnosis and were still alive and well. He made the road smoother.
Three days later, I had a shredding emergency, and between clients at Solo Bace, Steve Roy shaved my head as I cried like a baby. Steve’s colleague held my hand throughout, bless her.
There was no reconciling the woman in the mirror with my own perception of my self. I pulled a white knit beanie I had at the ready over my head, feeling ashamed.
Just as I got out of the chair, Emily arrived by taxi. She saw my red and puffy eyes, my beanie. “Aw, mum!” she said, hugging me. “How about dinner in Chinatown?” In our family, the answer to “Can we go to Chinatown?” is always “yes.”
Plus, I figured that the chances of running into someone I knew at Swatow were very small.
As if I wasn’t traumatized enough by the baldness, a few days later, my left hand went numb. I immediately assumed it was psychosomatic. But the numbness didn’t go away.
Two days later, there was something wrong with my left foot. It was numb, too.