I was diagnosed with breast cancer on March 18, 2013.
Ten days later, I had a lumpectomy and sentinel node biopsy, a procedure to remove the lymph nodes closest to the affected breast. All but one node tested positive for cancer, and the cancer had spread outside the lymph nodes as well.
Although the tumor was relatively small (1.7 cm), lymph node involvement meant the cancer was Stage IIIa.
I was 47, fit and active, and otherwise very healthy. I had no risk factors.
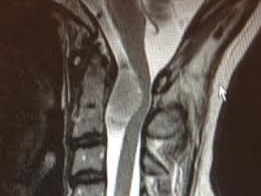
Six weeks later, on the day before my first chemotherapy treatment, my oncologist informed me that a full spine MRI revealed a benign but large (2.4 cm) tumor compressing my spinal cord between the first and second cervical vertebrae, just beneath my skull.
I was referred to a neurosurgeon who specializes in spinal cord tumours.
A few weeks after the nuerosurgery consult, I started losing sensation in my limbs. Each day, another part of an appendage went numb. Chemotherapy was interrupted for life-saving neurosurgery.
Post-chemotherapy, on November 14, I had an axillary lymph node dissection, the removal of a large rectangle of tissue under the arm. As was the case with my sentinel node biopsy, all but one node tested positive. And the cancer had spread extensively outside the nodes, in spite of four months of chemotherapy. It is not a typical finding, and since I was–and still am–symptom free, I was stunned by the pathology report.
Until that point, I had been handling the diagnosis exceptionally well, convinced that if other women had beat this disease, I can.
After a week of freaking out, I thought back to a conference I had attended in May: the International Health Promoting Hospitals and Health Services Network of the World Health Organization, which took place in Gothenburg, Sweden.
The theme of the conference was Body and Mind. One of the streams of the conference was psychoneuroimmunology (PNI), the study of the relationship between mental processes and the nervous and immune systems.
A paper on PNI was presented at the opening plenary session. I went to Sweden to present a paper at a W.H.O. conference–a lifetime achievement for me–but during that presentation realized I was meant to be there, to hear that message.
The connection between mind and body, between mental health and physical health, has been around for centuries, but in recent decades, researchers have confirmed that mental health status has a direct impact on immune response–at the cellular level. That is, the body’s ability to resist or rid itself of disease is impacted by one’s psychological health. Poor mental health status may compromise the body’s ability to deal with ailments from infections to chronic diseases, including cancer.
I’ve complied fully with the treatment regimen recommended by the teams at Princess Margaret Cancer Centre, as well as best advice from alternative care practitioners. Nevertheless, part of my body was full of carcinoma.
My goal is to control what I can.
How to improve my mental health status? Here’s what I’m already doing:
- Spending time with people I love
- Exercising
- Having sex
- Meditating
- Working with a psychotherapist
- Listening to music
- Singing
- Sleeping well
- Laughing as often as possible
- Making time for activities I love
I’m making a commitment to do much more of all of the above, and add anything else that causes endorphins to be released into my blood, or anything that makes me smile. I will also explore brain-training exercises to reduce the levels of cortisol (a hormone released in response to stress) and reach deeper levels of mindful meditation.
This site will document my quest to improve my mental health with an aim to condition my immune function and, by extension, optimize my outcomes.
I will also use this space to document my medical experience, which has been more of an acid trip than a “journey.” Welcome!
Related articles
- 8 Tips to Boost Your Immune System (leroyross754.wordpress.com)
- Build a Better Brain for Better Mental Health (psychologytoday.com)